Plantar warts are growths on the bottom of the foot caused by a virus that enters through small breaks in the skin. They can feel like stepping on a pebble and may become painful with pressure. Treatment depends on size, number, and how long they have been present. Over-the-counter options may help in early cases, but stubborn warts often need professional care. A podiatrist may use methods such as freezing, topical medications that break down the tissue, or gentle removal of thickened skin to reduce discomfort and improve treatment success. Sometimes more than one visit is needed, as these growths can be persistent. Keeping the area clean, dry, and protected can also support healing. If you notice a painful spot on the bottom of your foot that does not go away, it is suggested that you see a podiatrist for a proper diagnosis and appropriate care.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Dr. David Ungar from Personal Foot Care. Our doctor will assist you with all of your foot and ankle needs.
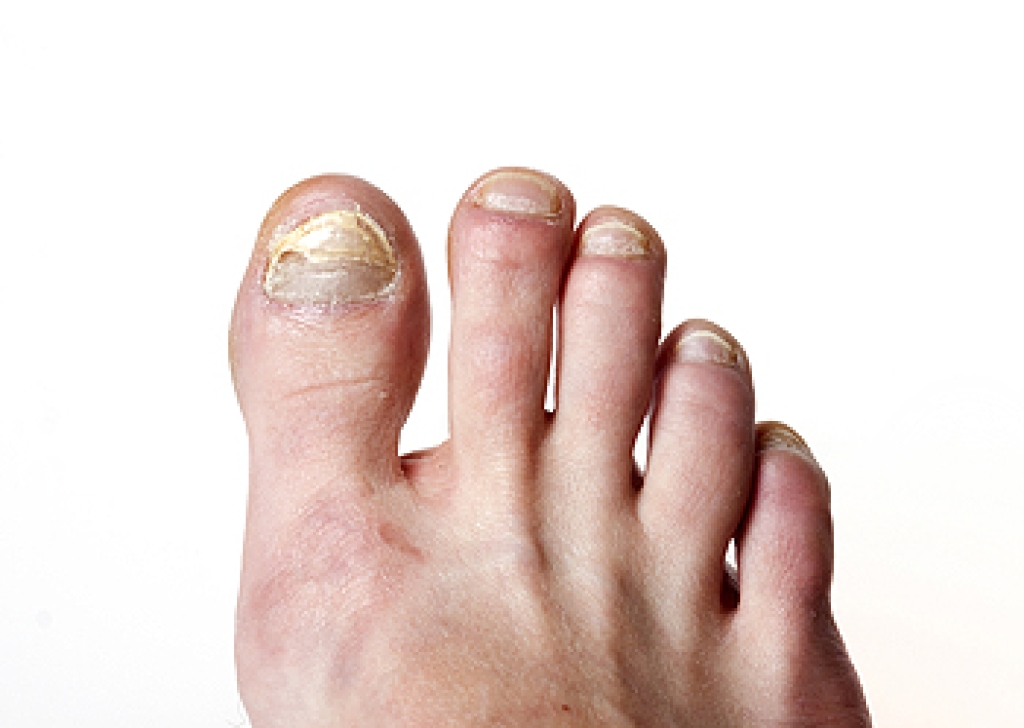
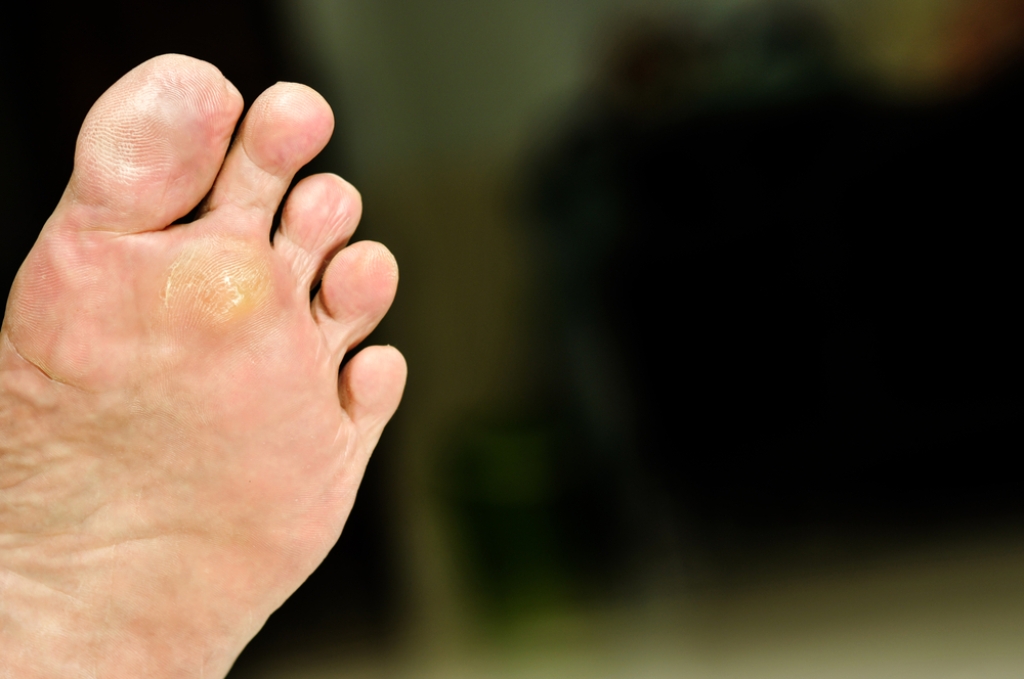
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions, please feel free to contact our office located in Farmington, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.