We practice a minimally invasive approach to your foot or ankle problem with surgery as the last option
An ingrown toenail is a nail that has curved downward and grows into the skin. This typically occurs at the nail borders, or the sides of the nail. As a result, pain, redness, swelling, and warmth may occur in the toe. If a break in the skin forms due to the ingrown nail, bacteria may enter and cause an infection in the area; this is typically characterized by a foul odor and drainage.
Ingrown toenails have multiple reasons for developing. In many instances, the condition is a result of genetics and is inherited. The most common cause, however, is improper trimming; cutting the toenails too short forces the skin beside the nail to fold over. An ingrown toenail can also develop due to trauma, such as stubbing the toe, having an object fall on the toe, or participating in activities that involve repeated kicking or running. Wearing shoes that are too tight or too short can also cause ingrown toenails.
Treatment for an ingrown toenail varies between patients and the severity of the condition. Milder cases that don’t involve infection or other medical conditions can benefit from soaking the feet in room-temperature water and gently massaging the side of the nail. In most cases, however, it is best to see your podiatrist for thorough and proper treatment. After examining your toe, your podiatrist may prescribe oral antibiotics to clear the infection if one is present. Surgical removal of either a portion of the nail or the entire nail may also be considered. In some cases, complete removal or destruction of the nail root may be required. Most patients who undergo nail surgery experience minimal pain afterward and can return to normal activity the following day.
Ingrown toenails can be prevented with proper nail trimming and by avoiding improper-fitting shoes. When cutting the toenails, be sure that you are cutting in a straight line and avoid cutting them too short. Shoes should not be too short or tight in the toe box.
 Ingrown toenails are uncomfortable and can sometimes make it painful to walk. Common causes for this condition include ill-fitting shoes, injury, excessively sweaty feet, and thick or curved nails. Once they have started to form, ingrown toenails can go through three stages. Stage 1 begins with the initial inflammation and is followed by moderate pain, swelling, redness, and visible fluid accumulation. Stage 2 occurs if the symptoms begin to worsen. Signs that the nail is entering stage 2 are increased pain and pus discharge from the wound. Stage 3 is the most severe form of an ingrown toenail and requires medical attention in order to be treated. In stage 3, new tissue can form over the wound, which can easily intensify the infection. It’s important to begin treating an ingrown toenail as soon as you notice any symptoms, so you can avoid progression into stage 3. If you have an ingrown toenail, it is recommended you consult with a podiatrist to learn about treatment options.
Ingrown toenails are uncomfortable and can sometimes make it painful to walk. Common causes for this condition include ill-fitting shoes, injury, excessively sweaty feet, and thick or curved nails. Once they have started to form, ingrown toenails can go through three stages. Stage 1 begins with the initial inflammation and is followed by moderate pain, swelling, redness, and visible fluid accumulation. Stage 2 occurs if the symptoms begin to worsen. Signs that the nail is entering stage 2 are increased pain and pus discharge from the wound. Stage 3 is the most severe form of an ingrown toenail and requires medical attention in order to be treated. In stage 3, new tissue can form over the wound, which can easily intensify the infection. It’s important to begin treating an ingrown toenail as soon as you notice any symptoms, so you can avoid progression into stage 3. If you have an ingrown toenail, it is recommended you consult with a podiatrist to learn about treatment options.
Ingrown toenails may initially present themselves as a minor discomfort, but they may progress into an infection in the skin without proper treatment. For more information about ingrown toenails, contact Dr. David Ungar of Personal Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails are caused when the corner or side of a toenail grows into the soft flesh surrounding it. They often result in redness, swelling, pain, and in some cases, infection. This condition typically affects the big toe and may recur if it is not treated properly.
Causes
You are more likely to develop an ingrown toenail if you are obese, have diabetes, arthritis, or have any fungal infection in your nails. Additionally, people who have foot or toe deformities are at a higher risk of developing an ingrown toenail.
Symptoms
Some symptoms of ingrown toenails are redness, swelling, and pain. In rare cases, there may be a yellowish drainage coming from the nail.
Treatment
Ignoring an ingrown toenail can have serious complications. Infections of the nail border can progress to a deeper soft-tissue infection, which can then turn into a bone infection. You should always speak with your podiatrist if you suspect you have an ingrown toenail, especially if you have diabetes or poor circulation.
If you have any questions, please feel free to contact our office located in Farmington, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blisters are pockets of fluid that occur under the top layer of your skin. These fluid pockets are usually filled with pus, blood, or serum. Blisters may itch or hurt and can appear as a single bubble or in clusters.
The most common types of blisters are friction blisters. This type of blister may be caused by wearing shoes that are too tight. Friction blisters can also occur on the hands. A change in temperature may also cause blisters on the feet. In the freezing air, frostbite on your toes can lead to blisters, as well as sunburn from hot weather.
The best way to treat a blister is to keep it clean and dry. Most blisters will get better on their own. Once the skin absorbs the fluid within the blister, it will flatten and eventually peel off. You should avoid popping your blister unless you podiatrist does it for you. Additional treatment options include applying an ice pack to the blister or using over-the-counter blister bandages to cover the affected area.
If your blister becomes discolored, inflamed, or worsens it is advised that you speak to your podiatrist. Blisters that are yellow, green, or purple may be infected and require immediate medical attention. Blisters that are abnormally colored may be a sign of a more serious underlying health condition such as herpes.
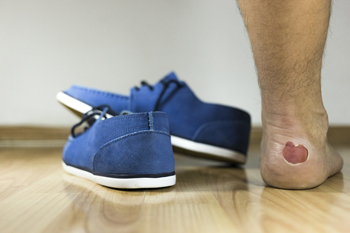 Patients who have suffered from blisters are familiar with the pain and discomfort they may cause. They may develop as a result of increased friction on a portion of the skin, which may come from wearing shoes or socks that fit improperly. When the skin becomes exposed, a blister will form as part of the body’s natural defense mechanism. This consists of a pocket of fluid which protects the affected area of skin. Additional reasons why blisters may develop may include allergic reactions to a bee sting or insect bite, or neuropathy which may originate from diabetes. If neuropathy is present, it may cause the patient to be unaware of existing blisters, and this may be a result of the inability to sense discomfort. When new skin begins to grow under the blister, it will generally drain on its own. If you have a blister on your foot that has become infected, it is suggested to speak to a podiatrist who can properly assist you in obtaining the correct treatment.
Patients who have suffered from blisters are familiar with the pain and discomfort they may cause. They may develop as a result of increased friction on a portion of the skin, which may come from wearing shoes or socks that fit improperly. When the skin becomes exposed, a blister will form as part of the body’s natural defense mechanism. This consists of a pocket of fluid which protects the affected area of skin. Additional reasons why blisters may develop may include allergic reactions to a bee sting or insect bite, or neuropathy which may originate from diabetes. If neuropathy is present, it may cause the patient to be unaware of existing blisters, and this may be a result of the inability to sense discomfort. When new skin begins to grow under the blister, it will generally drain on its own. If you have a blister on your foot that has become infected, it is suggested to speak to a podiatrist who can properly assist you in obtaining the correct treatment.
Blisters may appear as a single bubble or in a cluster. They can cause a lot of pain and may be filled with pus, blood, or watery serum. If your feet are hurting, contact Dr. David Ungar of Personal Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters are often the result of friction. This happens due to the constant rubbing from shoes, which can lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
Symptoms
(Blister symptoms may vary depending on what is causing them)
Prevention & Treatment
In order to prevent blisters, you should be sure to wear comfortable shoes with socks that cushion your feet and absorb sweat. Breaking a blister open may increase your chances of developing an infection. However, if your blister breaks, you should wash the area with soap and water immediately and then apply a bandage to the affected area. If your blisters cause severe pain it is important that you call your podiatrist right away.
If you have any questions, please feel free to contact our office located in Farmington, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Heel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.
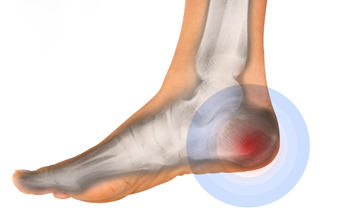 Many patients suffer from heel pain, and there may be several reasons why this may occur. These may include injuries to the foot that involves the heel, chronic conditions such as plantar fasciitis, bruises or stress fractures. Achilles tendonitis may develop as result of overuse, which may happen while participating in sporting activities. A heel pad bruise may occur as a result of wearing shoes that do not have adequate cushioning. It may also occur from falling from a high distance and landing on the heel. A condition that is known as haglund’s syndrome may occur if a bony protrusion develops on the back of the heel as it rubs against shoes that are stiff. Symptoms of this may include pain in the heel area of the foot, and possible swelling. If you are experiencing any type of heel pain, it is strongly suggested that you seek the counsel of a podiatrist who can properly diagnose and treat heel pain.
Many patients suffer from heel pain, and there may be several reasons why this may occur. These may include injuries to the foot that involves the heel, chronic conditions such as plantar fasciitis, bruises or stress fractures. Achilles tendonitis may develop as result of overuse, which may happen while participating in sporting activities. A heel pad bruise may occur as a result of wearing shoes that do not have adequate cushioning. It may also occur from falling from a high distance and landing on the heel. A condition that is known as haglund’s syndrome may occur if a bony protrusion develops on the back of the heel as it rubs against shoes that are stiff. Symptoms of this may include pain in the heel area of the foot, and possible swelling. If you are experiencing any type of heel pain, it is strongly suggested that you seek the counsel of a podiatrist who can properly diagnose and treat heel pain.
Many people suffer from bouts of heel pain. For more information, contact Dr. David Ungar of Personal Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions, please feel free to contact our office located in Farmington, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
 Overuse of the muscles in the feet may lead to a condition that is known as stress fractures. This may occur when the muscles undergo repeated impact which may result in a tiny fracture in the bone. The majority of stress fractures occur in the metatarsals, which is the portion of the foot that is thinner and longer, and bears the most weight while walking or running. Additionally, this type of fracture may occur in the heel or on top of the foot. It may be prevalent among people who may change or suddenly increase the intensity of their workout, or from wearing shoes that fit improperly. There are patients who may have medical conditions which may include osteoporosis. This may weaken the bones, and performing daily activities may prove to be difficult. If you have endured a stress fracture, it is suggested to consult with a podiatrist who can properly treat this condition.
Overuse of the muscles in the feet may lead to a condition that is known as stress fractures. This may occur when the muscles undergo repeated impact which may result in a tiny fracture in the bone. The majority of stress fractures occur in the metatarsals, which is the portion of the foot that is thinner and longer, and bears the most weight while walking or running. Additionally, this type of fracture may occur in the heel or on top of the foot. It may be prevalent among people who may change or suddenly increase the intensity of their workout, or from wearing shoes that fit improperly. There are patients who may have medical conditions which may include osteoporosis. This may weaken the bones, and performing daily activities may prove to be difficult. If you have endured a stress fracture, it is suggested to consult with a podiatrist who can properly treat this condition.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact Dr. David Ungar from Personal Foot Care. Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our office located in Farmington, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Connect With Us
